Before and After
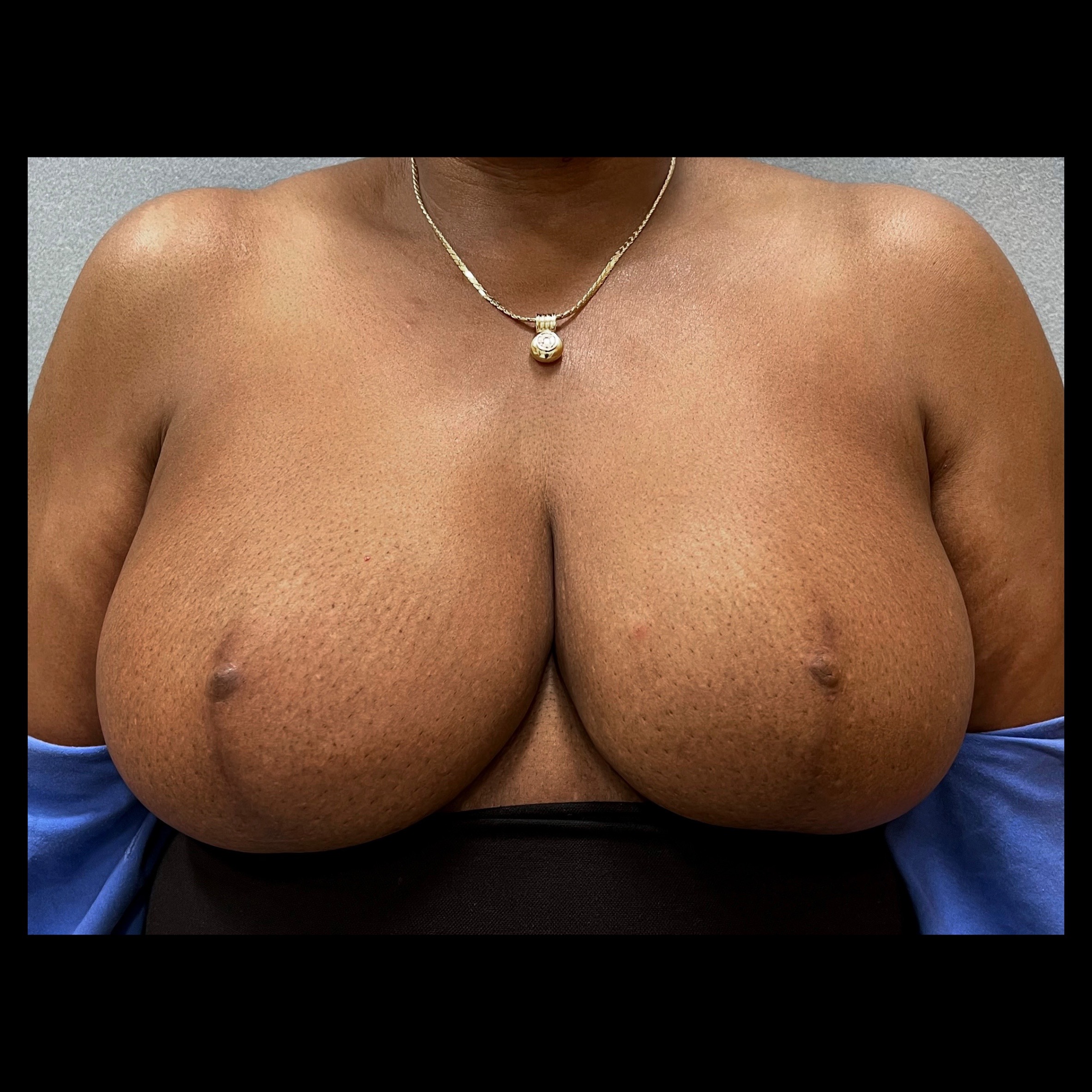
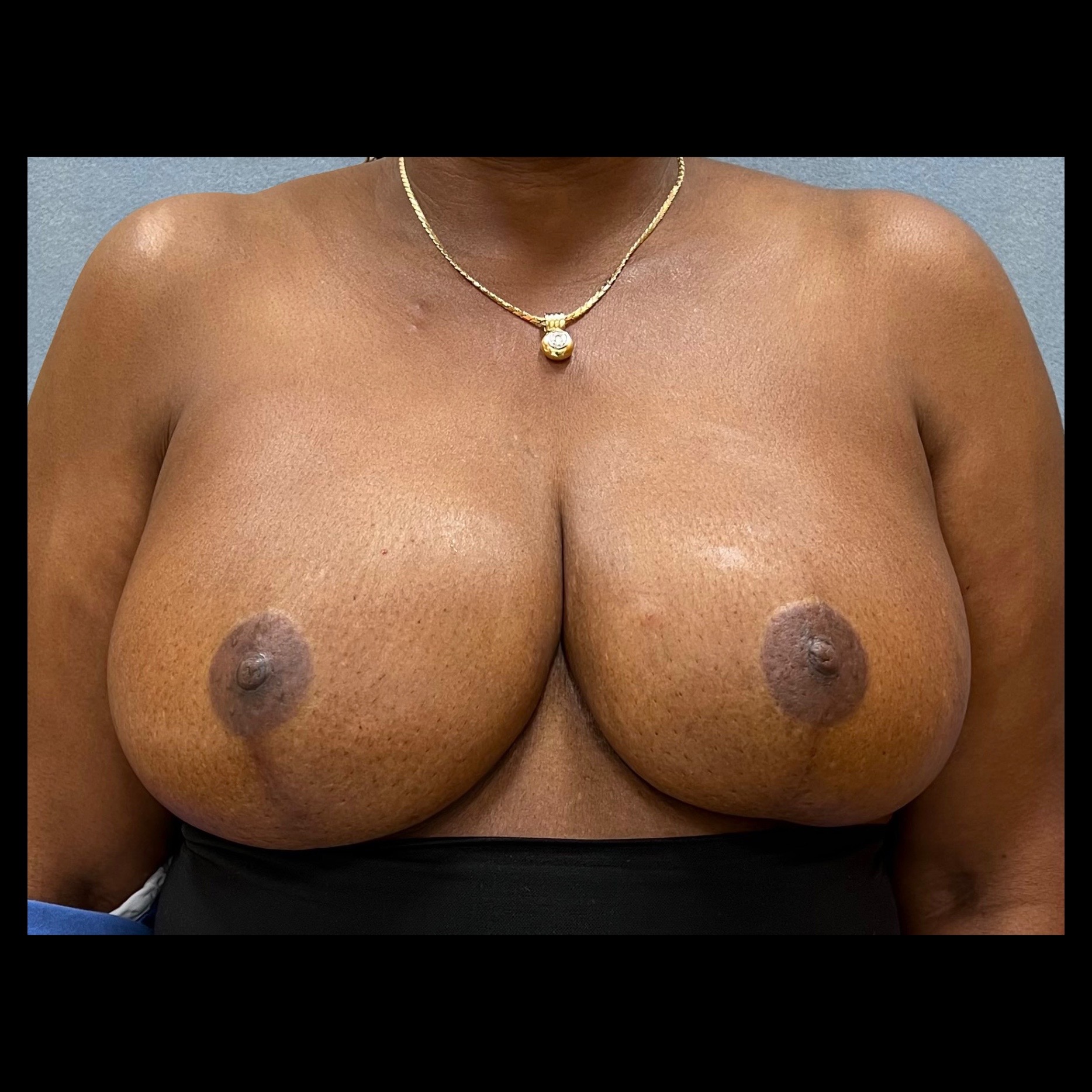
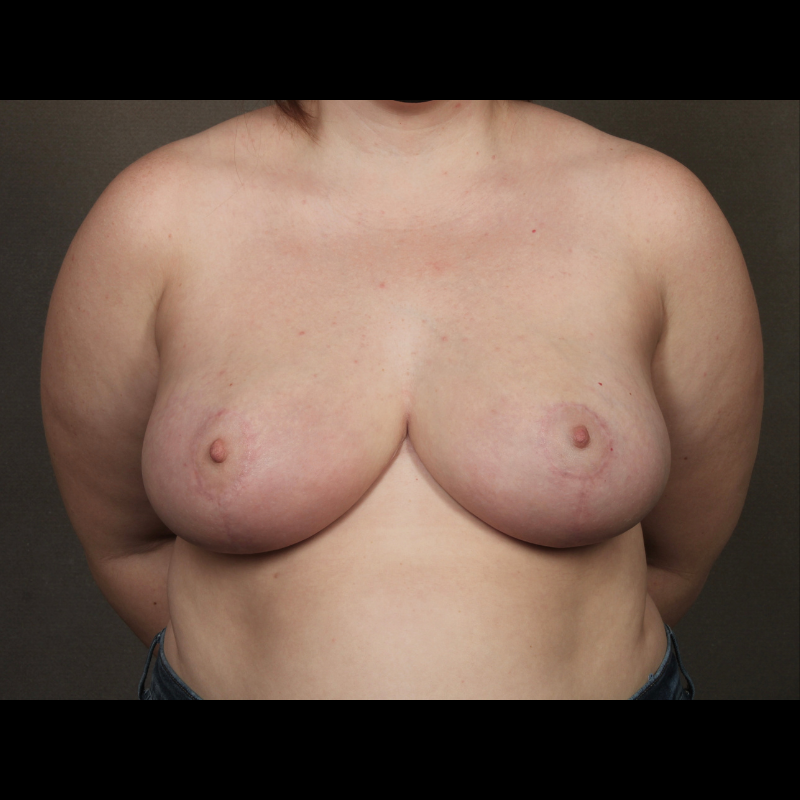
Breast Reduction
Breast reduction decreases breast size while reshaping breast contour and elevating nipple position. Symptoms related to large breast size, including neck pain, back pain, and recurrent rashes underneath the breasts, can improve after breast reduction.
See Full Gallery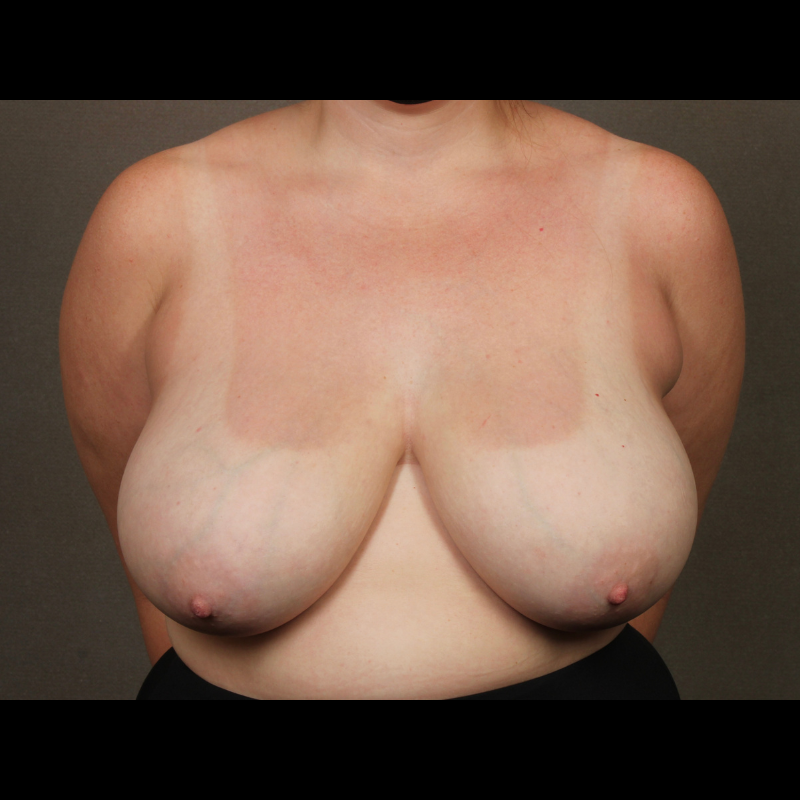
Breast Reconstruction
Diep Flap: Skin Sparing Mastectomy
With this combination of techniques, the nipple areola is removed along with breast glandular tissue, while the remaining breast skin is preserved during mastectomy. Then, a flap of skin and fat from the lower abdomen is transplanted to the chest wall.
See Full Gallery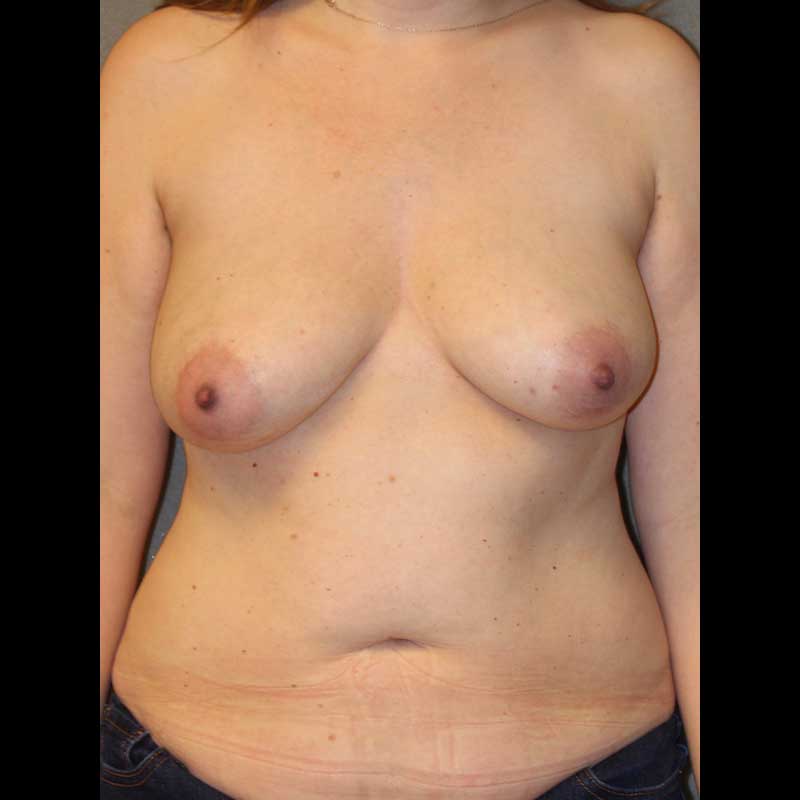
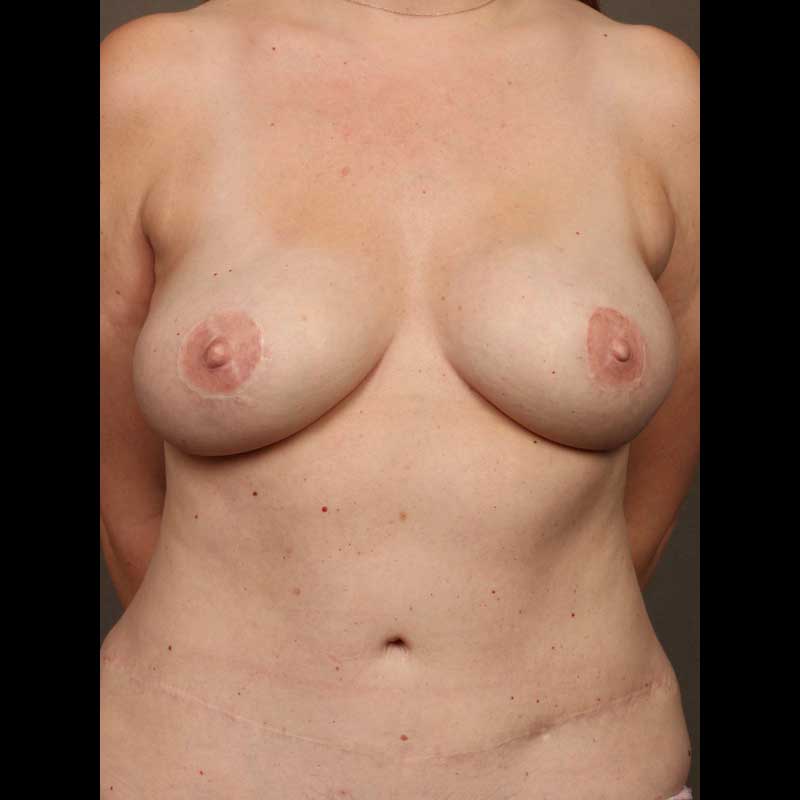
Breast Reconstruction
Diep Flap: Nipple Sparing Mastectomy
In these cases, the nipple areola is left intact along with the remaining breast skin, and only the breast glandular tissue is removed during mastectomy. Then, a flap of skin and fat from the lower abdomen is transplanted to the chest wall.
See Full Gallery![Case 7 Color photo of ]Breast Reconstruction DIEP Flap](https://nybra.com/wp-content/uploads/2020/03/hn-pre-1-wbg.jpg)
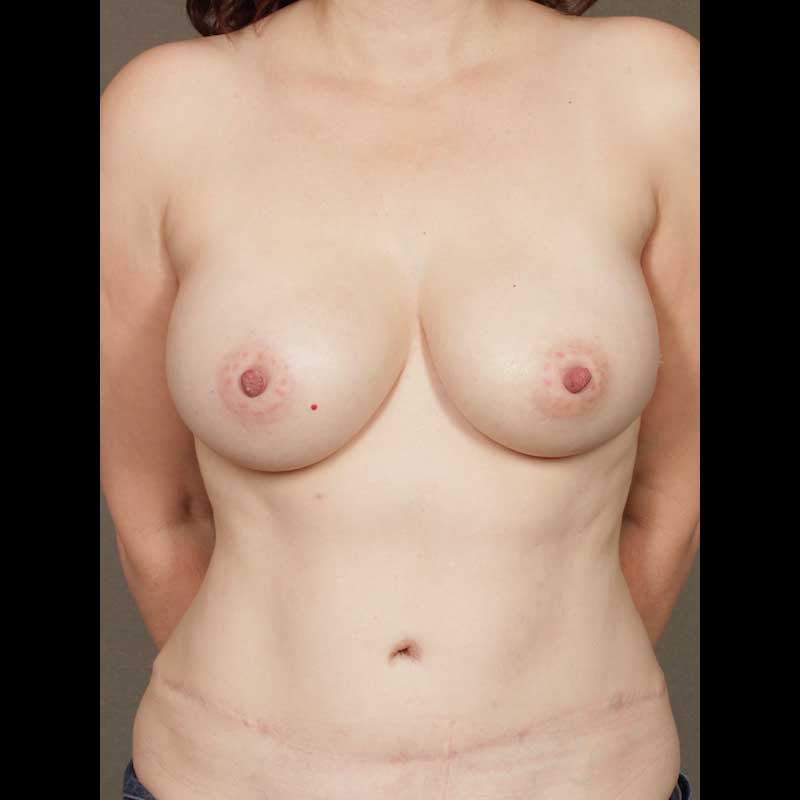
Breast Reconstruction
Diep Flap: Delayed Reconstruction
Women in this section underwent mastectomy, followed by DIEP flap reconstruction during a later, second stage procedure. DIEP flap reconstruction involves transplanting a flap of skin and fat from the lower abdomen to the chest wall.
See Full Gallery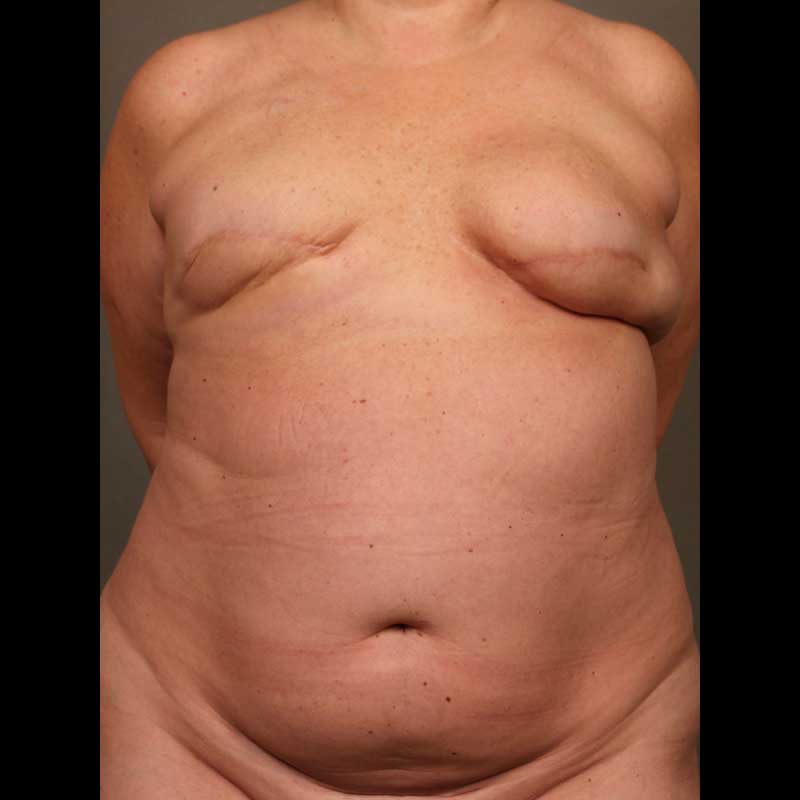
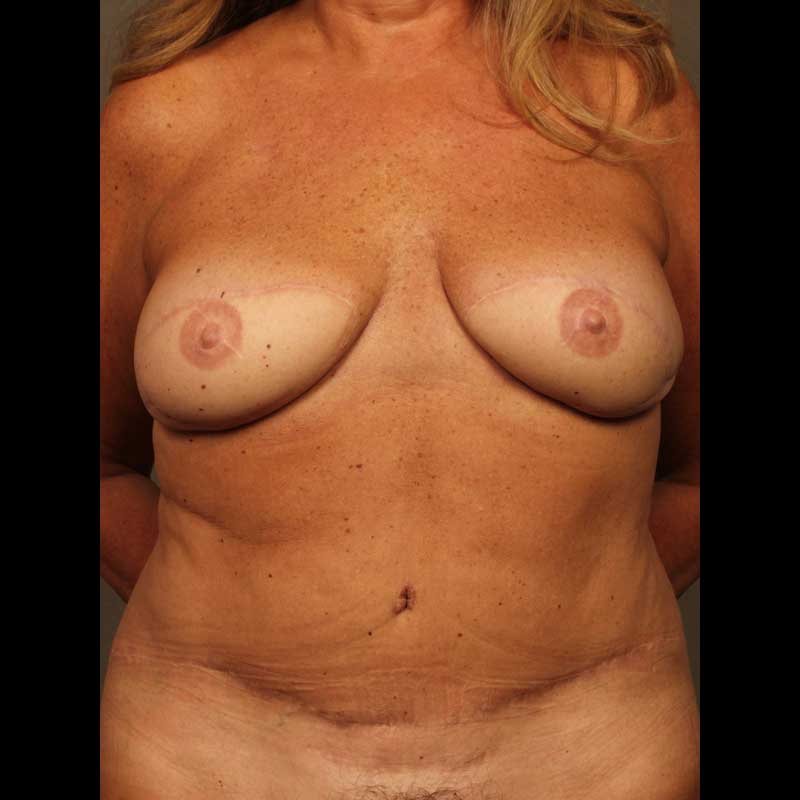
Breast Reconstruction
TUG/PAP Flap
In this natural-tissue flap reconstruction technique, fatty tissue is transplanted from the inner thigh to the chest wall to create a breast. Pioneered by a NYBRA surgeon, the fleur-de-lis TUG flap and PAP flap extends the option of natural tissue reconstruction to women who may not be ideal candidates for DIEP flap reconstruction.
See Full Gallery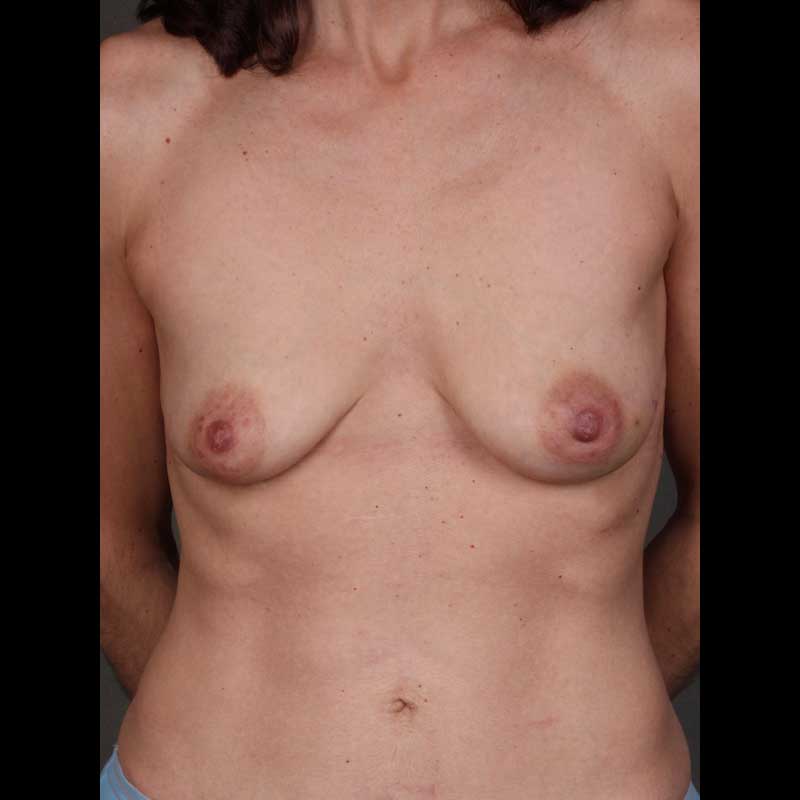
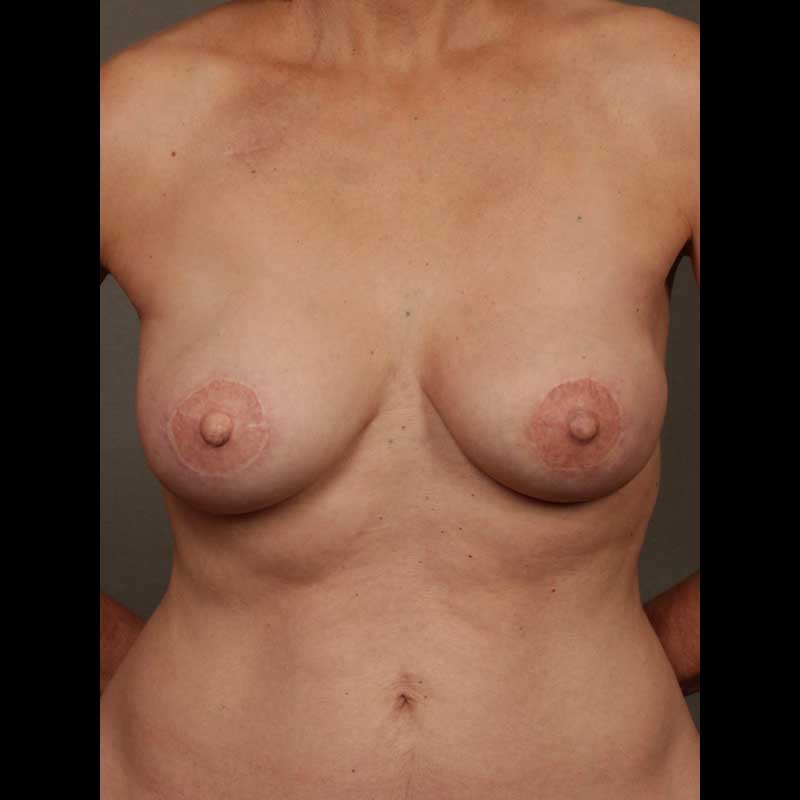
Breast Reconstruction
Latissimus Flap: Skin Sparing Mastectomy
This combination of techniques removes the nipple areola along with breast glandular tissue, while preserving remaining breast skin during mastectomy. Then, the latissimus dorsi muscle and skin from the back are transferred to the chest wall to create a breast. In most cases, this flap is placed over a breast implant.
See Full Gallery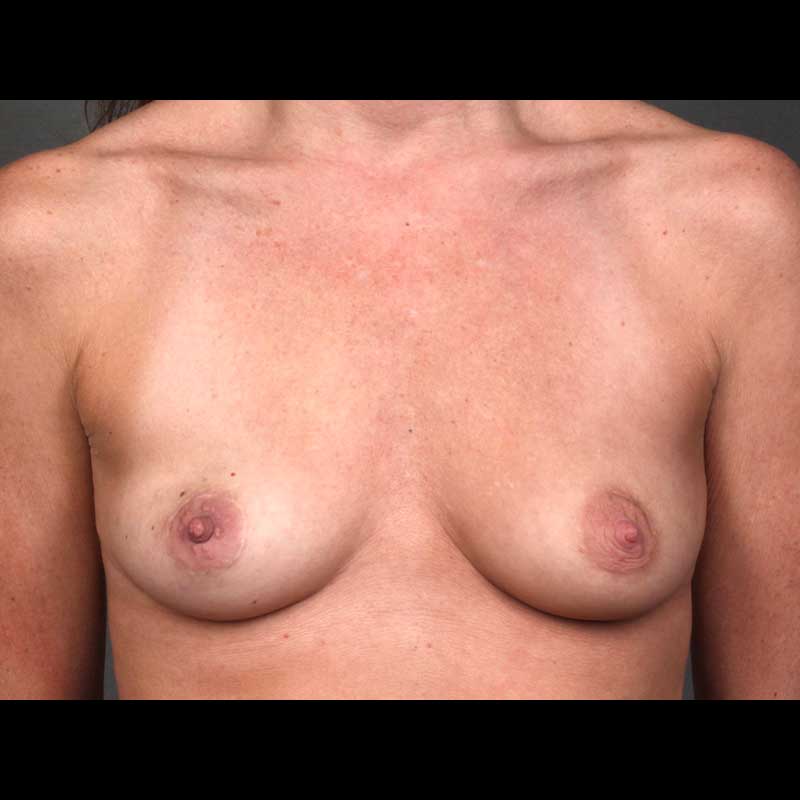
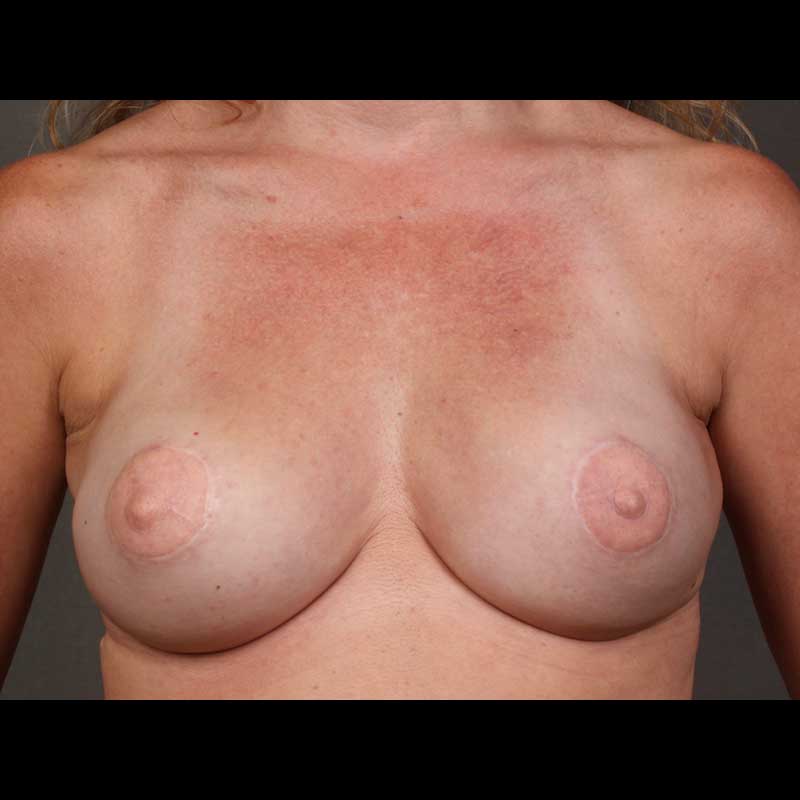
Breast Reconstruction
Latissimus Flap: Delayed Reconstruction
In these cases, the latissimus dorsi muscle and skin from the back were transferred to the chest wall to create a breast during a second stage operation. This can be done to correct partial mastectomy defects or to salvage unsatisfactory outcomes from prior implant or other flap breast reconstruction procedures.
See Full Gallery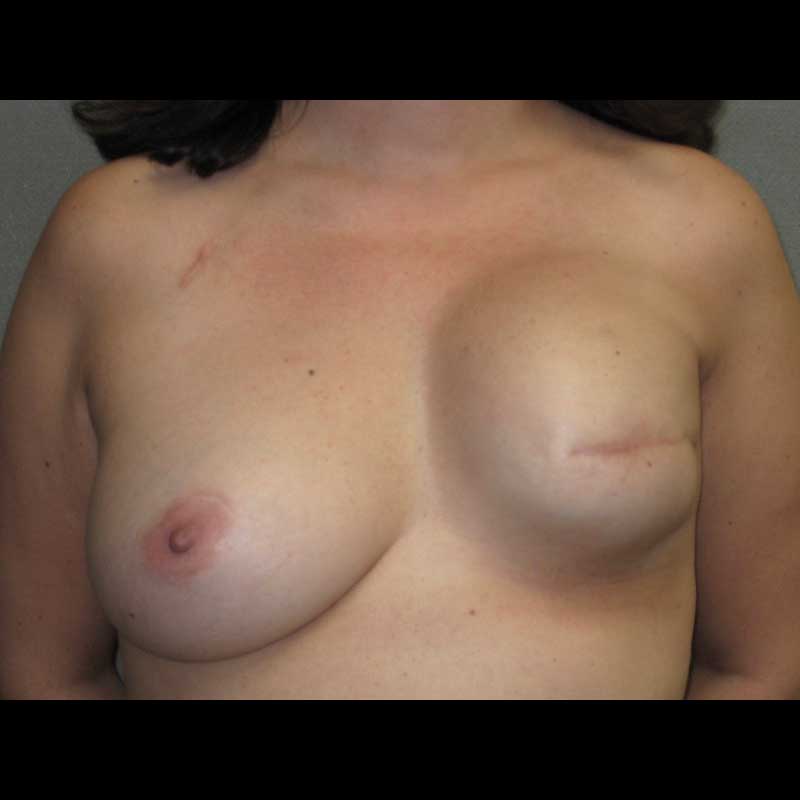
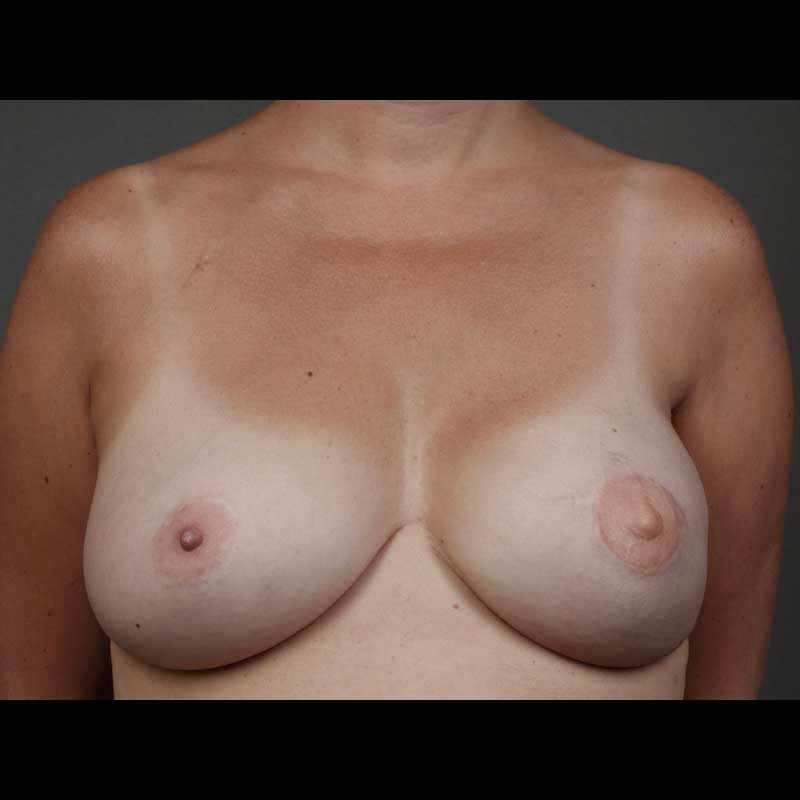
Breast Reconstruction
Direct to Implant: Nipple Sparing Mastectomy
In these cases, the nipple areola is left intact along with the remaining breast skin, and only the breast glandular tissue is removed during mastectomy. Then, our surgeons place a breast implant immediately, without using a tissue expander.
See Full Gallery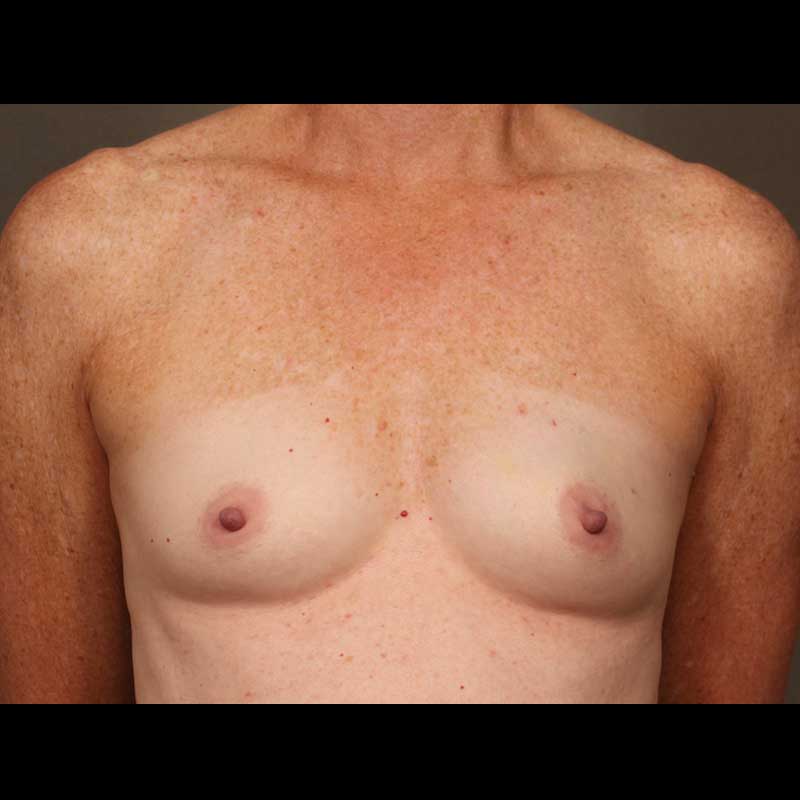
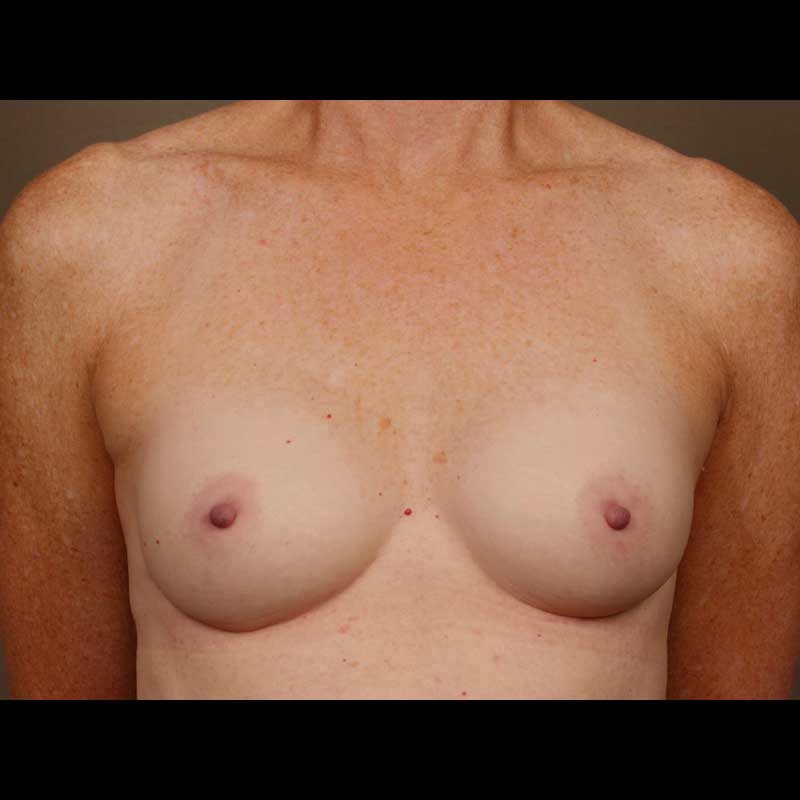
Breast Reconstruction
Expander Implant: Nipple Sparing Mastectomy
With this combination of approaches, the nipple areola is left intact along with the remaining breast skin, and only the breast glandular tissue is removed during mastectomy. Then, a tissue expander is placed. The expander is exchanged for a final implant during a later, second stage procedure.
See Full Gallery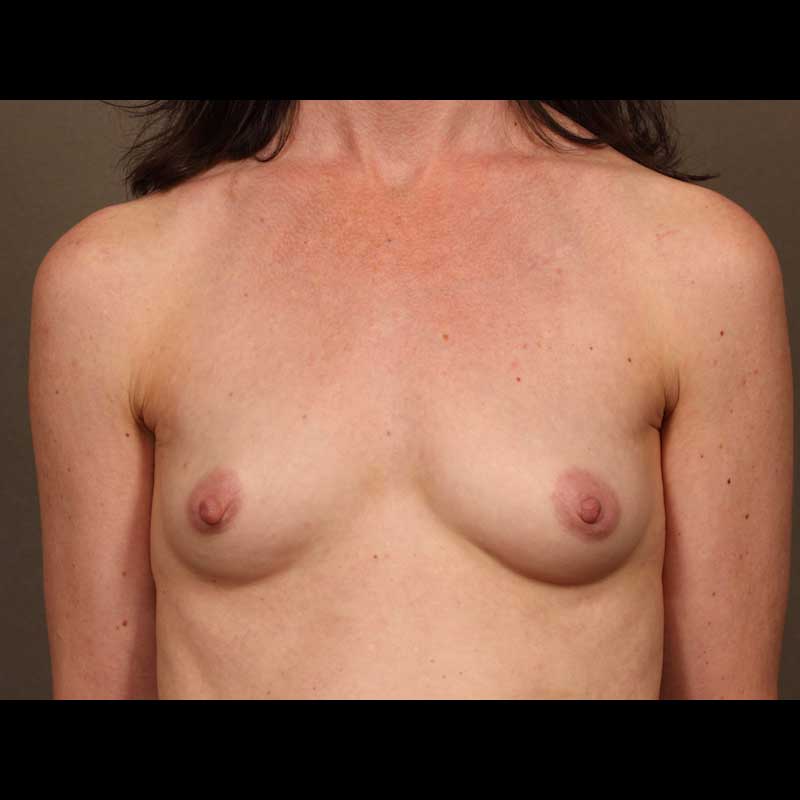
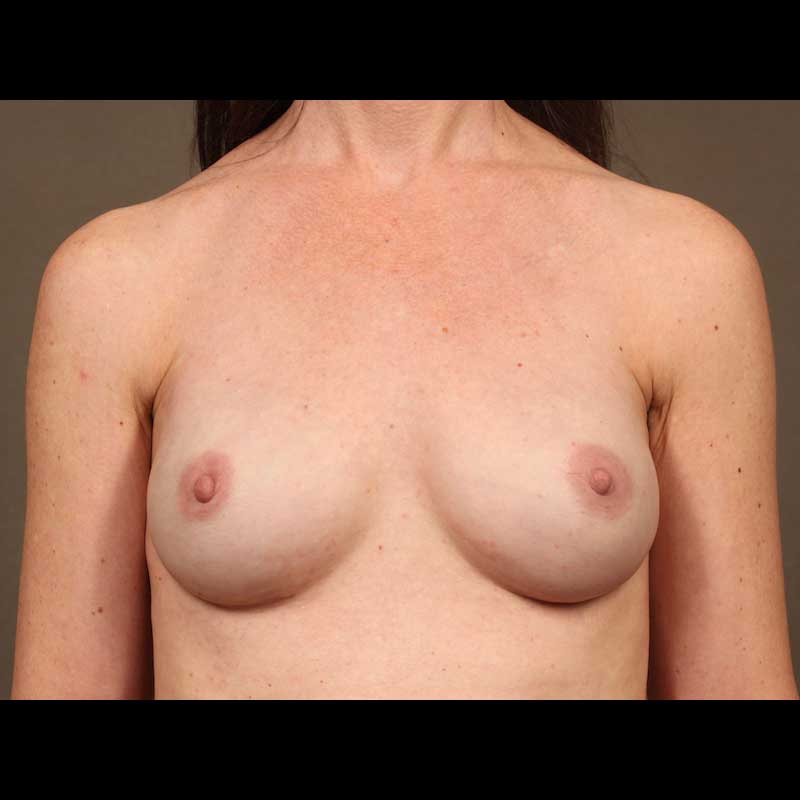
Breast Reconstruction
Expander Implant: Skin Sparing Mastectomy
With this combination of techniques, the nipple areola is removed along with breast glandular tissue, while the remaining breast skin is preserved during mastectomy. Then, an expander implant is placed. The expander implant is exchanged for a final implant during a later, second stage procedure.
See Full Gallery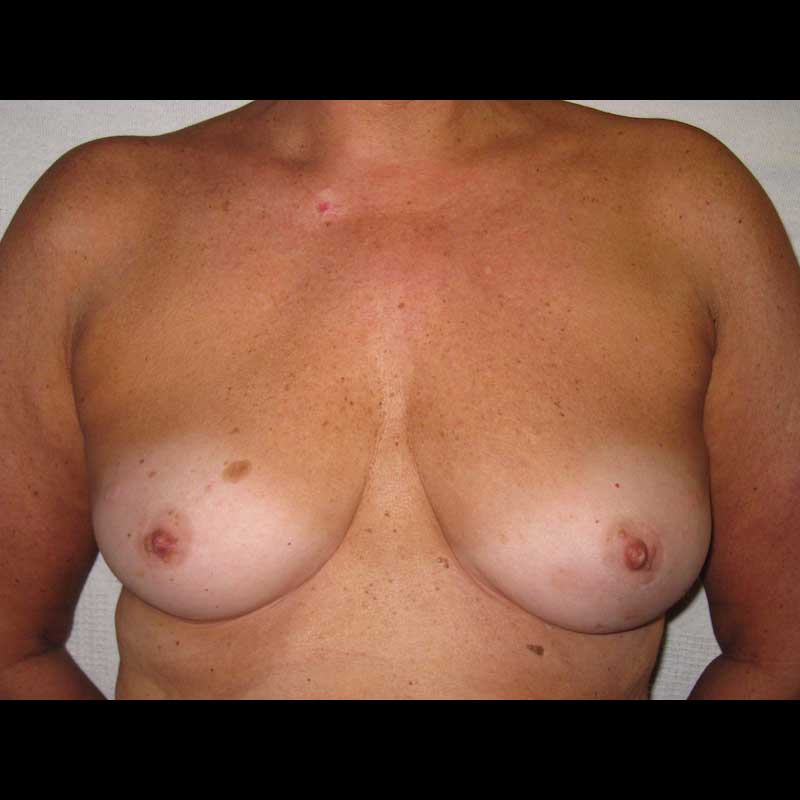
Breast Reconstruction
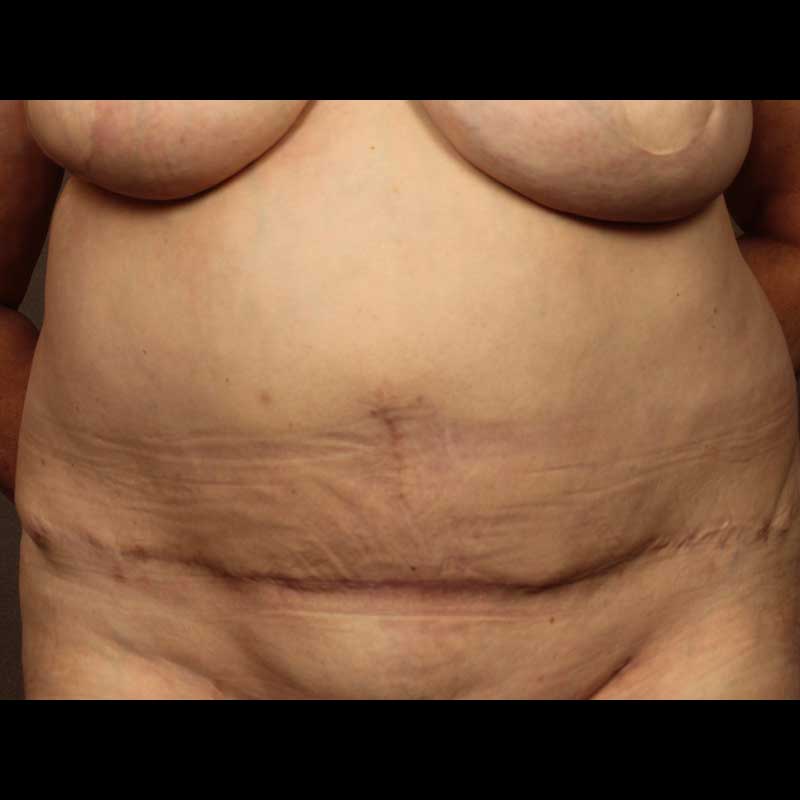
TRAM Hernia Repair
Women who have had traditional pedicled TRAM flap breast reconstruction risk developing lower abdominal weakness and contour deformities. While many are told that they have little recourse, we pioneered a unique and reliable abdominal wall reconstruction procedure to repair TRAM flap related hernias a contour deformities.
See Full Gallery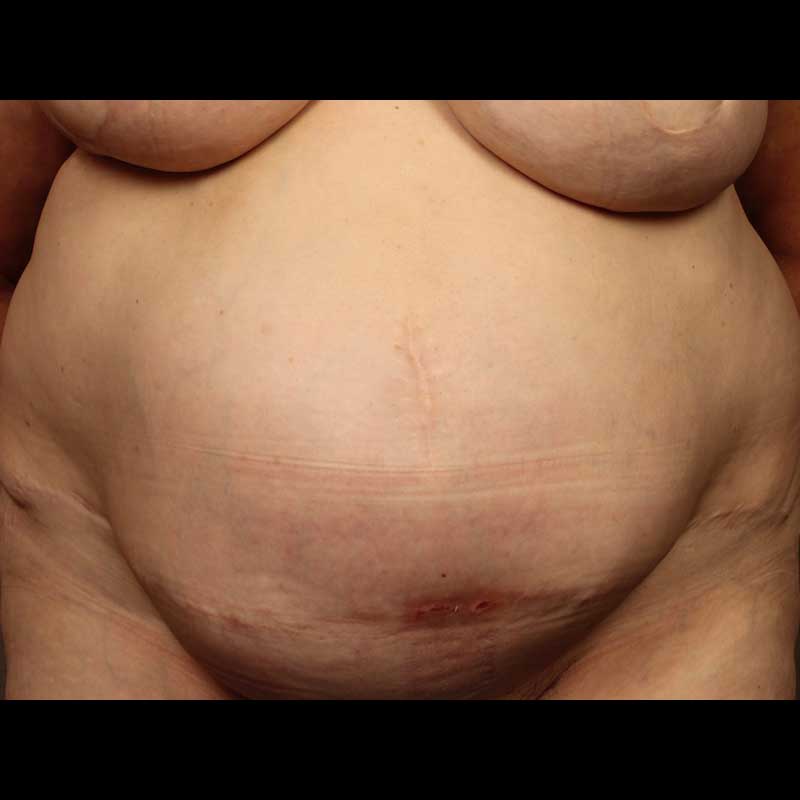
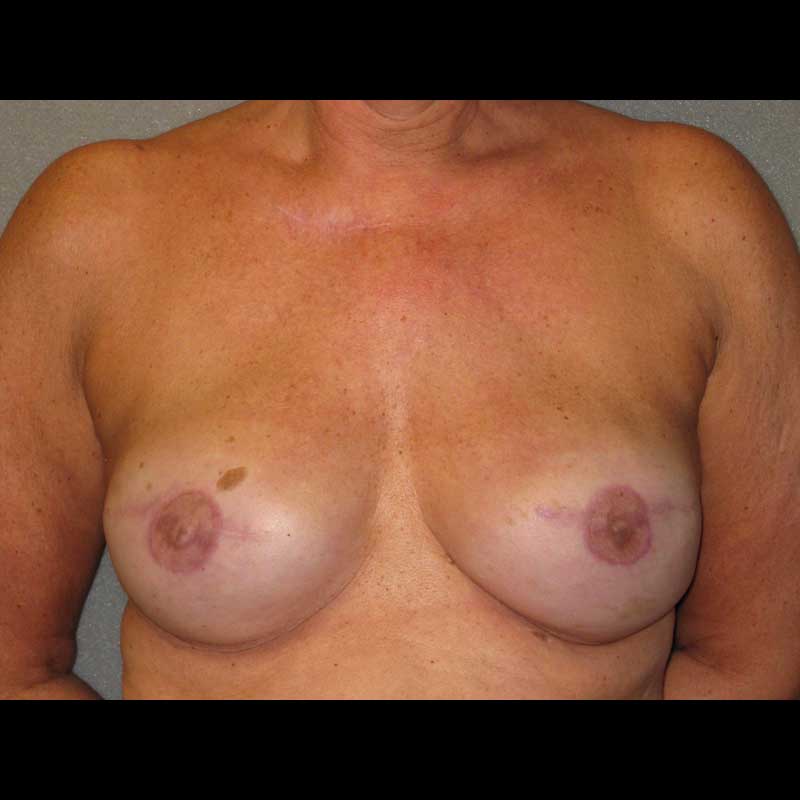
Restorative Tattoo
Nipple Tattoo
Tattooing adds natural nipple areola color to the final breast reconstruction. In some cases, tattooing alone can create the appearance of a three dimensional nipple.
See Full Gallery